Introduction
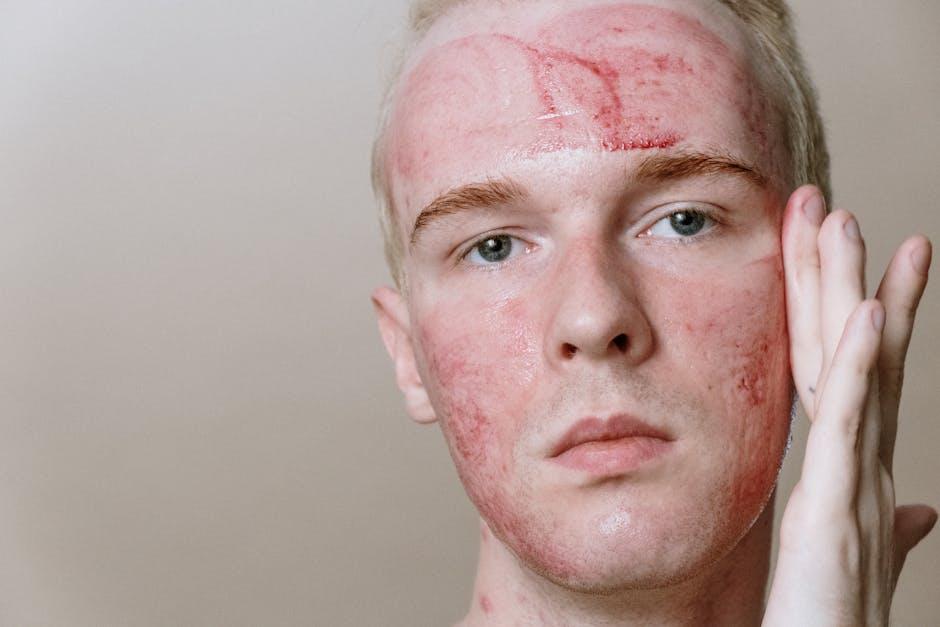
Niacin, also known as vitamin B3, is an essential water-soluble vitamin crucial for human health, involved in numerous metabolic pathways, including energy production, DNA repair, and cellular signaling. Despite its therapeutic role in lipid management and the prevention of pellagra, niacin has garnered notoriety for a distinct side effect: skin flushing, characterized by redness, warmth, itching, and tingling sensations, predominantly affecting the face and upper body. Understanding this reaction is vital for clinicians, patients, and the broader public health community, as niacin is readily available in dietary supplements, prescription formulations, and fortified foods. Notably, individuals with heightened sensitivity may experience severe or distressing symptoms that can undermine adherence too therapy or cause unwarranted concern. This article provides an exhaustive, evidence-based exploration of niacin-induced flushing, elucidating its mechanisms, clinical implications, risk factors, and management strategies.
What Is Niacin (Vitamin B3)?
Niacin encompasses two forms: nicotinic acid and nicotinamide (niacinamide), each with distinct biological activities and side effect profiles. As an indispensable micronutrient, niacin supports over 400 enzymatic reactions, primarily as the precursors to nicotinamide adenine dinucleotide (NAD) and its phosphate derivative NADP, wich are key cofactors in oxidative and reductive biochemical reactions. deficiency leads to pellagra—a once-common condition characterized by dermatitis, diarrhea, dementia, and, if untreated, death. Therapeutically, niacin’s cholesterol-lowering properties have led to its use in dyslipidemia, though its side effects often limit utility [NIH Office of Dietary Supplements].
- Recommended Dietary Allowance (RDA): Adult males: 16 mg NE/day; adult females: 14 mg NE/day (NE: Niacin equivalents).
- Dietary sources: Meat, fish, poultry, enriched breads, cereals, legumes, and seeds.
- Supplemental and pharmacological forms: Immediate-release, extended-release, sustained-release niacin, and non-flushing variants such as niacinamide.
for additional information on niacin’s functions and requirements, visit the MedlinePlus Niacin entry.
Overview of Niacin Flushing
Skin flushing is a well-recognized and dose-dependent pharmacological reaction following niacin governance, manifesting as a transient erythema (redness) with associated warmth or tingling. This phenomenon is especially pronounced with immediate-release (IR) formulations, while sustained-release and niacinamide rarely induce flushing due to thier metabolic and pharmacokinetic differences [Mayo Clinic].
Clinical Presentation and Symptomatology
- Onset: Typically occurs 15–30 minutes after ingestion, peaking within 1 hour, and resolving in 1–2 hours.
- Distribution: Predominantly affects the face, neck, upper thorax, and arms.
- Symptoms: Redness, warmth, burning, itching, or tingling sensations. Severe reactions may be accompanied by dizziness, headache, or hypotension.
- Resolution: symptoms are transient and rarely persist beyond several hours.
See the NCBI StatPearls article on Niacin for a concise review.
Why Does Niacin Cause Skin Flushing?
The dermatological manifestations observed after niacin ingestion are primarily vasodilatory, resulting from a complex interplay of biochemical mediators. The principal mechanism involves the G-protein coupled receptor GPR109A, which is activated by high concentrations of nicotinic acid in skin Langerhans cells. Activation of this receptor triggers the release of prostaglandin D2 (PGD2) and,to a lesser extent,prostaglandin E2 (PGE2)—potent vasodilators responsible for the characteristic flush [The Lancet].
- Pathophysiology: Niacin → GPR109A activation in skin → Prostaglandin release → Vasodilatation → Flushing
- Genetic factors: Variants in the PTGDR (prostaglandin D2 receptor) and genes modulating prostaglandin synthesis may contribute to individual susceptibility [NCBI – Genetic studies].
- Other mediators: Histamine release is minimal,evidenced by poor efficacy of antihistamines in attenuating niacin flush.
Notably, niacinamide—a related form—does not cause flushing due to differential receptor affinity and metabolic pathways [PubMed].
Prevalence and Risk Factors: Who Is Sensitive to Niacin Flushing?
Studies estimate that up to 90% of individuals taking pharmacological doses (≥500 mg/d) of immediate-release niacin experience some degree of flushing [JAMA Cardiology]. While mild, transient flushing is common and benign, a subset of individuals—classified as sensitive—report more intense or bothersome reactions.
- Formulation and dosage: Immediate-release niacin and higher doses dramatically increase flushing risk.
- Genetic predisposition: Single-nucleotide polymorphisms (SNPs) in prostaglandin pathway genes may confer heightened sensitivity [NCBI].
- Age and gender: Older adults and females may have a greater propensity for vasodilatory reactions.
- comorbid conditions: Individuals with cardiovascular disease, atopic disorders, or mast cell activation may report exacerbated symptoms.
- concurrent medications: Certain antihypertensive or vasodilatory drugs may potentiate flushing via additive effects.
- Alcohol and hot beverages: Consumption around the time of niacin intake can intensify flushing.
Importantly, while cutaneous flushing is distressing, it rarely signals a perilous or allergic reaction.
The Differential Diagnosis: Distinguishing Niacin Flushing from Allergy and Other Causes
Understanding the clinical characteristics of niacin flushing is imperative to differentiate it from allergic reactions or other dermatoses. While niacin flushing is an expected pharmacologic side effect,niacin allergy (immunoglobulin E-mediated hypersensitivity) is exceedingly rare and typically presents with urticaria,angioedema,or anaphylactic features.
| Feature | Niacin Flushing | Allergic Reaction |
|---|---|---|
| Onset | 15–30 min after ingestion | usually within minutes; variable |
| Distribution | Face, neck, upper torso | Diffuse; may include lips, eyelids |
| Symptoms | Warmth, redness, tingling, itching | Urticaria, swelling, airway symptoms |
| duration | Self-limited (1–2 hrs) | Variable; may require intervention |
| Systemic findings | Rare | Possible hypotension, respiratory distress |
For more on medication allergies, see the NHS allergy resource.
Epidemiology: How Common Is Niacin Flushing?
The incidence and severity of niacin flushing depend on both dosage and formulation. Key epidemiological findings include:
- IMMEDIATE-RELEASE NIACIN: Upwards of 80–90% of patients report flushing at therapeutic lipid-lowering doses.
- EXTENDED/SUSTAINED-RELEASE: Formulations reduce but do not eliminate flushing (estimated incidence 20–50%) [PubMed].
- NON-FLUSHING NIACINAMIDE: Practically no incidence of flushing for standard therapeutic regimens.
- SENSITIVE POPULATIONS: True intolerance—marked by therapy discontinuation or severe symptoms—ranges from 5–20% across studies.
Self-reporting biases and underrecognition may influence prevalence estimates, particularly outside clinical trial settings.
Pathophysiology: the Role of Prostaglandins and Skin Receptors
Niacin flushing represents a prototypical example of prostaglandin-mediated vasodilation. When niacin is ingested, especially in its immediate-release form, large quantities enter the systemic circulation and interact with GPR109A receptors located on Langerhans cells and keratinocytes in the dermis. The sequence of molecular events is:
- Niacin binds to GPR109A (also called HM74A or HCAR2) on skin immune cells.
- Activation of this receptor stimulates phospholipase A2.
- Arachidonic acid release leads to cyclooxygenase (COX)-mediated conversion to prostaglandins, predominantly PGD2 and PGE2.
- Prostaglandins bind to their respective EP and DP receptors on dermal blood vessels.
- Resulting vasodilation increases blood flow, manifesting clinically as erythema and sensation of warmth.
A notable clinical fact is that pharmacologic blockade of cyclooxygenase with aspirin prior to niacin dosing greatly attenuates flushing by limiting prostaglandin synthesis [harvard Health Blog].
Clinical Implications: Is Flushing Dangerous?
While often uncomfortable, niacin-induced flushing is considered a benign and predictable pharmacodynamic effect. Still, for a subset of sensitive individuals, flushing might potentially be profound, engendering anxiety, disrupting daily activities, or prompting discontinuation of therapy—undesirable in those who benefit from niacin’s lipid-lowering effects. Importantly, true complications are rare.
- no link to anaphylaxis: Unlike drug allergies, flushing does not progress to airway compromise or systemic collapse.
- Transient hypotension: Rare in high-sensitivity individuals,mainly at very high doses or with comorbid cardiovascular instability.
- Adherence impact: Severe or intolerable flushing can undermine adherence to prescribed regimens, compromising cardiovascular risk reduction.
Healthcare providers are encouraged to differentiate between benign flushing and hypersensitivity, providing patient reassurance and education.
Managing Niacin-Induced Flushing: Clinical Strategies
A range of evidence-based approaches exist to minimize flushing without sacrificing therapeutic efficacy for those requiring niacin treatment. These include formulation choice, dose titration, adjuvant pharmacotherapy, and patient education.
Formulation Modification
- Extended-release or sustained-release niacin: Associated with significantly reduced incidence and severity of flushing due to slower systemic absorption [FDA].
- Inositol hexanicotinate: Marketed as “flush-free,” but has questionable efficacy in raising HDL or reducing LDL; clinical effectiveness differs [Medical News Today].
- Niacinamide (nicotinamide): Does not cause flushing and is appropriate for deficiency prevention but lacks hypolipidemic effects.
Initiation and Dose Titration
- Start at the lowest possible dose, gradually titrating upwards (e.g., 100–250 mg/day increased weekly) to minimize abrupt prostaglandin release.
- take with meals to further attenuate gastrointestinal absorption and acute plasma peaks.
Pharmacologic Prophylaxis
- Aspirin (acetylsalicylic acid): Pre-treatment with 30–60 mg 30 minutes prior to niacin dosing attenuates flushing in most individuals by inhibiting cyclooxygenase and prostaglandin synthesis [NCBI – clinical trial].
- nsaids (ibuprofen): May offer similar prostaglandin suppression.
- Antihistamines: Generally ineffective, supporting the non-histaminergic nature of niacin flushing.
Lifestyle and Behavioral Adjustments
- avoid ingestion on an empty stomach or with hot beverages/alcohol, which can exacerbate vasodilatory symptoms.
- Regular, consistent dosing may lead to tachyphylaxis, with tolerance to flushing developing over 1–2 weeks of continued therapy.
Patient Education and Counseling
- Explain the benign nature of flushing to reduce anxiety and improve therapeutic adherence.
- Warn patients about expected symptoms, onset, and duration to set realistic expectations.
- Encourage patients to contact clinicians if symptoms are intolerable or if unusual signs emerge (e.g., severe rash, swelling, signs of anaphylaxis).
A extensive review of management strategies can be found at Healthline’s guide on niacin flush.
Summary table: Flushing Risk by Niacin Formulation
| Formulation | flushing risk | Clinical Comment |
|---|---|---|
| Immediate-release niacin | Very high (80–90%) | Most pronounced, rapid onset |
| Extended-release niacin | Moderate (20–50%) | Prolonged absorption, reduced peak effect |
| Inositol hexanicotinate (“flush-free”) | Low | Limited evidence for lipid effects |
| Niacinamide (nicotinamide) | None | No flushing; lacks lipid-lowering effect |
Frequently Asked Questions (FAQs)
1. How can I prevent niacin flush?
Strategies include using extended-release formulations,slow dose titration,taking niacin with food,and pre-medicating with low-dose aspirin. Avoid hot drinks and alcohol with the dose.
2. Is niacin flush harmful?
No, niacin flush is a benign, self-limited reaction.Severe or persistent symptoms should prompt consultation, but life-threatening allergic phenomena are extremely rare.
3. Can “no-flush” niacin supplements raise HDL or lower LDL cholesterol?
Most “no-flush” supplements (inositol hexanicotinate) do not consistently confer cardiovascular benefits comparable to prescription niacin. Nicotinamide lacks hypolipidemic efficacy.
4. Which groups are most sensitive to niacin flushing?
Those with genetic predispositions, higher initial doses, or using immediate-release forms are most sensitive. Females, older adults, and individuals with certain comorbidities may also experience increased symptoms.
5. Should I stop niacin if I get flushed?
Mild to moderate flushes are expected and typically subside with regular dosing or mitigation strategies. Abrupt discontinuation is rarely necessary unless severe intolerance or other adverse effects arise. Always consult your healthcare provider before stopping any prescribed therapy.
Safety, Contraindications, and When to seek Medical Advice
While niacin-induced flushing is not generally dangerous, individuals should remain vigilant for possible adverse effects and absolute contraindications.
- Liver dysfunction: High-dose niacin can cause hepatotoxicity, particularly with sustained-release forms. Regular monitoring of liver enzymes is advised during therapy [CDC].
- Gout and hyperuricemia: Niacin can elevate plasma uric acid levels.
- Peptic ulcer disease: May exacerbate gastric irritation.
- Severe flushing with systemic symptoms: Seek care if flushing is accompanied by difficulty breathing, chest pain, or swelling of the tongue/lips—these are not typical features and may signal an allergic or systemic reaction.
Routine side effects rarely require emergency intervention, but personalized risk stratification and patient-centered counseling are essential.
Current Research and Future Directions
Recent advancements have improved our understanding of niacin flushing at the molecular level, particularly the identification of skin GPR109A receptors as therapeutic and side effect targets. Ongoing clinical trials are evaluating receptor-specific antagonists, new slow-release delivery platforms, and combinatorial therapies (e.g., with laropiprant, a PGD2 receptor blocker) to optimize cardiovascular benefits while minimizing adverse effects [NCBI – Future therapies].
research also explores pharmacogenetic predictors of sensitivity, aiming toward individualized niacin therapy based on genetic profiles, and the advancement of innovative “flush-free” prescription formulations for dyslipidemia.
Conclusion
niacin-induced flushing is a frequent, dose-dependent, and benign reaction rooted in prostaglandin-mediated vasodilatation, not allergy. Sensitive individuals may experience more pronounced symptoms, but strategic formulation choice, careful titration, premedication, and behavioral modifications can substantially reduce the incidence and impact of flushing. Most importantly, clear patient education and appropriate risk communication enhance adherence, safety, and therapeutic outcomes. For those experiencing intolerable reactions or considering niacin therapy, consultation with a healthcare professional is recommended for personalized advice and monitoring.
For further reading and up-to-date clinical guidance, refer to:
- Mayo Clinic: Niacin (oral route)
- NIH ODS Factsheet: Niacin
- Healthline: What’s a Niacin Flush?
- FDA: Niacin Drug Safety
References
- NIH office of Dietary Supplements. Niacin Fact Sheet.
- NCBI. The mechanism of niacin-induced flushing and potential therapies.
- Harvard Health Blog. The Niacin Flush.
- Mayo Clinic. Niacin (Oral route).
- U.S.FDA.Niacin Information.
- NCBI StatPearls. Niacin.
- PubMed. Extended-release niacin and flushing.
- Healthline. Niacin flush: How to prevent it and what it means.
- Medical News Today. What is niacin flush?
- NCBI. Genetic studies on niacin flushing.
- NHS. Allergic reaction overview.
- CDC.Occupational Health Guideline for Niacin.

