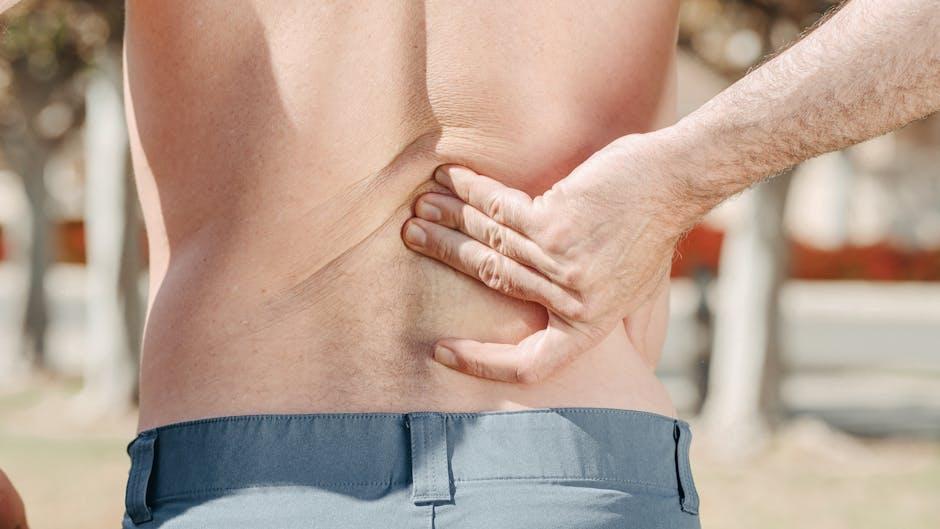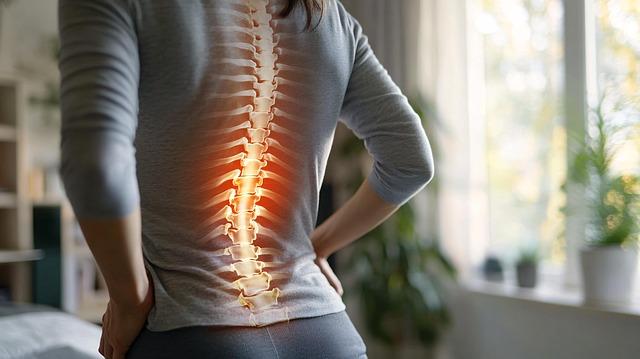
Lower back pain linked to long hours of sitting
Introduction
Lower back pain associated with prolonged periods of sitting has emerged as one of the most prevalent musculoskeletal complaints in modern society. According to the World Health Organization (WHO), musculoskeletal disorders, including lower back pain, represent the leading contributor to disability worldwide. In the United States alone, nearly 39% of adults report suffering from back pain within a three-month period (CDC). As a largely sedentary lifestyle characterized by long hours at desks and screens becomes more common, understanding the connection between sitting and lower back pain is critical for both public health and individual well-being. this article explores the epidemiology, underlying mechanisms, symptoms, diagnosis, and evidence-based strategies for prevention and management of lower back pain linked to long hours of sitting.
Overview and Definition
Lower back pain is defined as discomfort localized to the lumbar region, typically between the lower rib margins and the gluteal folds. It may present as acute, subacute, or chronic, depending on its duration (PubMed). The lumbar spine supports much of the body’s weight and is highly susceptible to biomechanical stress. Based on etiology, lower back pain may be classified as nonspecific (most cases), mechanical, or secondary to underlying pathology such as herniated disc, spinal stenosis, or systemic illness.
Epidemiological data indicates that approximately 80% of adults will experience lower back pain at least once in their lifetime (NIH: National Institute of Neurological Disorders and stroke).Chronic lower back pain—defined as pain persisting for more than 12 weeks—affects nearly 20% of those with acute episodes.Individuals between 30 and 50 years are most at risk, coinciding with the working-age population that tends to spend extensive hours in sedentary occupations.
From a pathophysiological perspective, lower back pain may involve muscular strain, ligamentous damage, intervertebral disc degeneration, or altered neural transmission. Prolonged sitting is increasingly recognized as a modifiable factor that can exacerbate these processes, underscoring the urgent need for public health awareness and preventive measures.
Causes and Risk Factors
The incidence and severity of lower back pain linked to long hours of sitting are influenced by a complex interplay of biological, genetic, behavioral, and environmental factors.Understanding these underlying mechanisms is essential for targeted interventions.
Prolonged Sitting and ural Stress
Extended sitting leads to ural imbalances, increased lumbar flexion, and sustained loading of intervertebral discs. This compressive force impairs disc nutrition,hastens degenerative changes,and may ultimately trigger pain due to mechanical and inflammatory pathways. Epidemiological studies confirm a positive correlation between sedentary behavior—particularly sitting for more than 6 hours daily—and prevalence of lower back pain (Harvard Health).
Slouched or unsupported sitting further increases the risk, as it places undue strain on the paraspinal muscles and erior spinal ligaments. Over time, these biomechanical alterations can manifest as both acute and chronic pain syndromes.
Muscle Inactivity and Deconditioning
Sedentary lifestyles contribute to weakening of the core stabilizing muscles, particularly the multifidus, erector spinae, and abdominal musculature. Evidence suggests that reduced muscle activity impairs spinal alignment and increases susceptibility to lumbar injury (PubMed). Deconditioning also diminishes ural endurance, exacerbating discomfort during prolonged static ures.
Intervertebral Disc degeneration
Cartilaginous intervertebral discs depend on intermittent movement for nutrient exchange and metabolic waste removal. When sitting restricts this dynamic loading, it accelerates dehydration and degeneration of the disc structure, heightening the risk of herniation and nerve root compression (Mayo Clinic).
Vascular and Neural Factors
Sustained sitting, especially with poor ure, can impede blood supply to the paraspinal tissues and compress peripheral nerves. For example, prolonged hip flexion may trigger sciatica or aggravate existing neuropathic conditions (Medical News Today). By impairing oxygenation and perfusion, these vascular changes also delay recovery in previously injured tissues.
Other Contributing Factors
- Age: Risk increases with advancing age due to disc degeneration and loss of spinal flexibility (NHS).
- Genetics: Familial predisposition may influence spinal anatomy and likelihood of degenerative conditions.
- Obesity: Excess body weight increases spinal loading, compounding the negative effects of sitting (CDC).
- Poor Ergonomics: Non-adjustable chairs,lack of lumbar support,and improper workstation setup heighten lumbar strain.
- Psychosocial Factors: Stress, job dissatisfaction, and mood disorders are linked with chronicity and higher pain perception (PubMed).
Anatomical illustration connecting prolonged sitting with the progress of lower back pain.
Pathophysiology: how Sitting contributes to Lower Back Pain
The relationship between extended sitting and lower back pain is grounded in the fundamental biomechanical and physiological changes that occur with static ure. Understanding these processes can inform clinical strategies for prevention and rehabilitation.
Spinal Loading and Disc Compression
Biomechanical research reveals that sitting increases intradiscal pressure compared to standing, particularly when lumbar support is absent. Every 20-degree loss in lumbar lordosis amplifies the mechanical force exerted on the spinal discs (PubMed). This repetitive compression creates microtrauma and hastens structural breakdown, setting the stage for pain and dysfunction.
Muscle Imbalance and Fatigue
Prolonged inactivity leads to selective atrophy of spinal stabilizing muscles while overactivating hip flexors and superficial back extensors. This imbalance disrupts spinal alignment and reduces the capacity for movement variability—a key factor associated with chronic pain (Harvard Health).
Circulatory and neural Dysfunction
Restricted movement during sitting impedes venous return, increases intracranial and intraspinal pressure, and may indirectly injure nerve roots. Ischemic changes, combined with mechanical irritation, often manifest as numbness, tingling, or radiating pain along the lower extremities (Mayo Clinic: Sciatica).
Inflammatory Mediators
Static sitting has been linked to elevated levels of pro-inflammatory cytokines, including TNF-α and IL-6. This chronic low-grade inflammation not only contributes to pain sensitization but may impede healing and increase the risk of chronic pain syndromes (JAMA).
Symptoms and Clinical Presentation
Lower back pain linked to prolonged sitting displays a spectrum of symptomatology:
- Dull, aching pain localized to the lower back
- Stiffness and loss of flexibility after periods of inactivity
- Radiation of pain into the gluteal region or lower extremities (rarely indicating nerve compression)
- Worsening pain with continued sitting; relief with standing or movement
- Occasional muscular spasms or tightness along the lumbar paraspinals
Chronic cases may involve psychological components—such as irritability or depressive symptoms—further complicating management (PubMed).
Diagnosis and Assessment
A thorough diagnosis requires careful clinical evaluation that includes medical history, physical examination, and, when warranted, advanced imaging.
Medical History and Patient Interview
Key aspects include occupational and lifestyle information, duration and character of symptoms, previous episodes, and red flag signs (such as recent trauma, unexplained weight loss, or neurological deficits) (Mayo Clinic).
Physical Examination
- Inspection for ural abnormalities, spinal alignment, and muscle tenderness
- Range of motion testing and neurological screening (strength, sensation, reflexes)
- Palpation to identify trigger points or muscle spasms
Diagnostic Imaging
routine imaging (X-ray, MRI, CT scan) is typically reserved for persistent, severe, or neurologically intricate cases (NHS).Most acute and nonspecific cases do not require imaging unless clinical suspicion of serious pathology is high.
Complications of Unmanaged Lower Back Pain
Chronic lower back pain, if left untreated, can progress to significant musculoskeletal and general health complications.
- Reduced mobility and diminished quality of life
- Loss of workforce productivity and increased absenteeism (The Lancet)
- Development of chronic pain syndromes including central sensitization
- Increased risk of anxiety and depression in chronic cases
- Secondary complications such as weight gain,cardiovascular risk,and deconditioning due to physical inactivity (CDC)
Prevention: Evidence-Based Strategies
Given that lower back pain from prolonged sitting is both pervasive and largely preventable, clinical guidelines emphasize multimodal interventions focusing on ergonomic adjustments, physical activity, and workplace health promotion (Healthline).
Ergonomics in the Workplace
- Maintain feet flat on the ground and knees at hip level
- Use chairs with adjustable lumbar support
- Align eyes with the upper third of the computer screen to minimize neck strain
- Position keyboard and mouse within arm’s reach to avoid excessive forward bending
Occupational health experts advise regular ergonomic assessments to optimize workstations and reduce cumulative strain.
Breaks and Micro-Movements
Healthcare guidelines recommend standing and moving for at least 5 minutes every 30–60 minutes of sitting (JAMA Network Open). Micro-breaks, stretching, or light walking can significantly alleviate muscle tension and boost spinal health.
Core Strengthening and Physical Activity
Structured exercise programs focusing on core stabilization, flexibility, and aerobic conditioning are proven to reduce the risk and burden of lower back pain (NIH).Yoga,Pilates,and physiotherapist-guided routines address both muscle balance and ural control.
Lifestyle Modification
- Weight management to decrease lumbar load
- Sufficient hydration and balanced nutrition for musculoskeletal health
- Stress reduction strategies to dampen pain amplification pathways
Treatment and Management
For those with established lower back pain, treatment must be individualized, adhering to the latest evidence-based protocols. Early, multidisciplinary intervention yields the best outcomes.
Non-Pharmacological Interventions
- Physical therapy: Manual therapy,McKenzie exercises,and core stabilization programs (Mayo Clinic).
- Heat/cold therapy: Soothes muscular tension and reduces acute pain.
- Cognitive behavioral therapy (CBT): Effective for chronic or refractory cases to address maladaptive pain behaviors (PubMed).
- Gradual return to activity: Encouraged as opposed to prolonged bed rest.
Pharmacological and Interventional Therapy
- NSAIDs and acetaminophen for short-term pain management (FDA).
- Muscle relaxants and neuropathic pain medications in select cases.
- Epidural steroid injections or nerve blocks for severe, refractory pain (MedlinePlus).
- Surgical intervention is reserved for cauda equina syndrome, intractable neurological deficits, or structural lesions unresponsive to conservative care (Harvard Health).
special populations and Considerations
Certain groups may require tailored approaches:
- Elderly: Vulnerable to osteoporosis, spinal stenosis, and comorbid conditions (NIH).
- Pediatric and adolescent populations: Increasing screen time and device use calls for age-appropriate ergonomic interventions (CDC).
- Pregnant women: Special attention to ure, pelvic support, and gentle exercise (NHS).
Current Research and Future Directions
Innovative studies continue to highlight the dangers of excessive sitting and the therapeutic benefits of movement, ergonomic technology, and behavioral change.Research into active workstations (e.g., sit-to-stand desks) shows promising effects on both musculoskeletal pain and metabolic health. Wearable devices that monitor ure and activity are increasingly used in occupational health settings to reinforce healthy behaviors.
Future clinical trials are focusing on the optimal composition, frequency, and intensity of physical activity necessary to offset sitting-related risks, as well as integrated digital and telemedical solutions for workplace prevention.
Frequently Asked Questions (FAQs)
- Can standing desks prevent lower back pain? – Evidence suggests that sit-to-stand desks can reduce back pain in some workers, but regular movement is still required (Harvard Health).
- How long is too long to sit without taking a break? – Experts recommend standing or moving at least every 30–60 minutes (Healthline).
- What is the best exercise for lower back pain? – Core stabilization, stretching, and aerobic activity are foundational; consult a physical therapist for personalized regimens (Mayo Clinic).
Conclusion
The strong scientific consensus is that extended periods of sitting are causally linked to the onset, persistence, and exacerbation of lower back pain. This relationship is mediated through biomechanical strain, muscular deconditioning, neurovascular compromise, and psychosocial factors. Given the overwhelming public health burden, both individuals and institutions must prioritize ergonomic design, active lifestyles, and early intervention. Employing evidence-based strategies—including workplace modifications, regular movement, and medical management—offers the best opportunity to mitigate risk, relieve suffering, and enhance quality of life for millions affected by lower back pain in today’s sedentary world.
For further guidance, consult your healthcare provider, physiotherapist, or occupational health specialist, and refer to resources from the world Health Organization, Centers for Disease Control and Prevention, and National Health Service (NHS).