 lower back pain“>
lower back pain“>
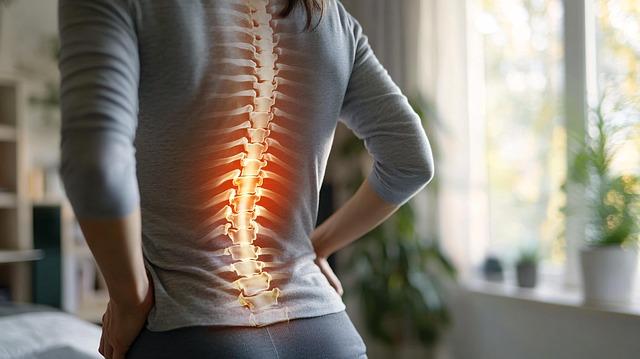
why lower back pain feels worse after resting too long
Introduction
Lower back pain is a global health issue affecting millions annually, with enormous socio-economic impacts and significant negative effects on quality of life. according to the World Health Organization (WHO), low back pain is the leading cause of disability worldwide, responsible for loss of productivity, healthcare costs, and individual suffering.The peculiar phenomenon where lower back pain feels worse after resting too long is frequently reported in clinical practice,often bewildering patients who assume rest should offer relief. Understanding this counterintuitive pattern is crucial for effective prevention, management, and rehabilitation of chronic and acute low back pain.
Research from the Centers for Disease Control and Prevention (CDC) reveals that up to 80% of adults experience low back pain at some point.Exploring the mechanisms behind worsening symptoms after inactivity or prolonged rest offers essential insight into both clinical care and patient self-management strategies, with implications for public health worldwide.
Overview and Definition
lower back pain, or lumbago, refers to discomfort, stiffness, or pain located within the lumbar region of the spine, specifically affecting structures such as the vertebrae, intervertebral discs, ligaments, muscles, and nerves. The condition is broadly classified into acute (lasting less than six weeks), subacute (lasting 6-12 weeks), and chronic (persisting for more than 12 weeks), as detailed by the National Institutes of Health (NIH).
the lumbar region bears a substantial portion of the body’s weight and enables foundational movements such as bending, lifting, and twisting.Epidemiological studies indicate that low back pain affects nearly 577 million people worldwide at any moment, with high recurrence rates and considerable heterogeneity in symptom experience.
Structurally, low back pain may stem from mechanical causes (e.g., muscle or ligament strain, herniated discs), degenerative diseases (such as osteoarthritis), inflammatory processes, infections, fractures, or referred pain from pelvic or abdominal organs. The impact extends beyond physical symptoms, contributing to psychological distress and limiting social and economic participation.
Causes and Risk Factors
Understanding why lower back pain can intensify after resting requires exploration of the multifactorial causes of low back pain and their interplay with inactivity. Below, we detail the main biological, genetic, environmental, and behavioral risk factors.
1.Musculoskeletal Dysfunctions
- Muscle Deconditioning: Prolonged inactivity leads to weakness and loss of endurance in back muscles, predisposing to pain during subsequent movement.According to the Mayo Clinic, deconditioned muscles are less capable of supporting the spine and absorbing shock.
- Ligamentous Laxity: During rest, ligaments supporting the vertebral column may stiffen or loose elasticity, contributing to morning pain or discomfort after prolonged sitting or lying.
2. Inflammatory and Metabolic Mechanisms
- Inflammatory mediators: Lack of movement allows pro-inflammatory cytokines (such as interleukin-1 and tumor necrosis factor-alpha) to accumulate, creating localized swelling and discomfort. Harvard Health explains the “morning stiffness” effect as partially due to inflammation pooling during sleep or prolonged rest.
- Reduced Blood Flow: Inactivity decreases circulation to affected tissues,delaying clearance of metabolic waste and inflammatory mediators,further sensitizing local pain receptors.
3. Neural Sensitization and Pain Perception
- Central Sensitization: Chronic pain can alter neurochemical processing in the spinal cord and brain, causing heightening of pain perception (hyperalgesia) after rest periods.
- Peripheral Sensitization: Nerves innervating the lumbar area may become hypersensitive during inactivity, leading to increased discomfort upon movement. This is particularly evident in patients with neuropathic low back pain,as discussed in a review published in the NIH database.
4. Disc Biomechanics and Hydration
- Disc Swelling: Intervertebral discs rehydrate during rest; this can increase disc bulge and compound discomfort after lying down or prolonged sitting, particularly in degenerative cases. This phenomenon is explained by the Spine-health resource.
5. Behavioral and Environmental Factors
- Sedentary Lifestyle: Extended immobility due to work, lifestyle, or recovery can perpetuate a cycle of pain and disuse.
- Poor Ergonomics: suboptimal sleeping surfaces or sitting ures during rest can strain lumbar tissues.
6. Age and Genetic Predisposition
Degenerative disc disease, osteoarthritis, and heritable abnormalities in connective tissue structure elevate risk for low back pain exacerbation during periods of inactivity, as analyzed in comprehensive cohort studies on low back pain epidemiology.
pathophysiological Mechanisms: Why Pain Worsens with Prolonged Rest
The exacerbation of lower back pain following inactivity stems from intricate physiological processes. Below, key mechanisms are outlined and supported by scientific research.
1. Muscle Atrophy and Weakness
Extended rest contributes to muscle atrophy, particularly of the paraspinal and core muscles responsible for spinal support. Weak musculature is less efficient in stabilizing the lumbar vertebrae, leading to increased susceptibility to strain upon resumption of activity. The International journal of Molecular Sciences identifies muscle wasting as a significant risk factor for persistent and activity-related low back pain.
2. Connective tissue Stiffness
Ligaments and fascia lose elasticity during long periods of inactivity, resulting in a stiff, less flexible lumbar spine. Stiffened ligaments increase resistance against movement, contributing to pain at the onset of mobility—especially recognizable as “morning stiffness” or “start-up pain.” NIH-backed evidence for this mechanism is summarized in connective tissue research.
3. Altered Inflammatory Response
Physical movement enhances lymphatic drainage and circulatory flow, facilitating the removal of inflammatory mediators from lumbar tissues. Conversely, immobility leads to their accumulation at sites of microscopic injury, perpetuating swelling and stimulating local nociceptors. This mechanism is substantiated in Harvard Health research.
4. Changes in Intervertebral Disc Pressure
while sleeping or lying down, intervertebral discs rehydrate and swell. In healthy discs,this is restorative; but in degenerative disc disease,increased morning disc height can exert pressure on adjacent nerve endings,aggravating symptoms upon rising. Medical News Today discusses this phenomenon and its relation to rest-associated discomfort.
5. Neural Sensitization
Persistent pain amplifies both central and peripheral sensitization, with inactivity compounding hypersensitivity states in the spinal cord and peripheral nerves. Studies confirm that patients with episodic or chronic low back pain report greater pain intensity after inactivity, as explored in review articles on pain sensitization.
6. Psychosocial Contributors
Rest, particularly enforced inactivity during injury or illness, may also evoke psychological responses—such as catastrophizing, depression, or anxiety—that exacerbate pain perception. The mind-body connection is outlined clearly by the Mayo Clinic,emphasizing the need for psychologically informed management strategies.
Epidemiology: Prevalence, Demographics, and Trends
low back pain is documented as the leading cause of years lived with disability among adults. Age,sex,occupation,and lifestyle behaviors all influence its prevalence and clinical characteristics.According to a comprehensive Lancet review, life-prevalence estimates for low back pain reach as high as 84%, with incidence peaking between ages 40 and 69. Occupational epidemiology highlights higher risks among laborers, drivers, and sedentary workers exposed to repetitive strain or prolonged static ures.
Several studies show that individuals with chronic low back pain are more likely to exhibit pain on waking, after sitting, or following periods of inactivity. These trends have profound impacts on work absenteeism, healthcare utilization, and long-term prognosis. Sociodemographic disparities exist, with older adults, women, and persons with lower socio-economic status reporting higher severity and chronicity of pain.
Symptomatology: Clinical Features Related to Inactivity
Pain related to prolonged rest has characteristic features distinct from other low back pain patterns:
- “Start-up” Pain: Acute discomfort upon initiating movement after inactivity (e.g., on waking or standing after sitting for extended periods).
- Stiffness: Sensation of rigidity or limited versatility, most marked in the early morning or after immobility.
- Localized Ache: Dull pain confined to the lumbar region, occasionally radiating to the buttocks or thighs.
- Transient Worsening: Pain or discomfort that eases after 15–30 minutes of gentle movement.
Recognition of these patterns is essential for prompt diagnosis and the differentiation of benign musculoskeletal pain from more serious pathologies (e.g., infection, fracture, malignancy), as explained by NHS guidance.
Diagnostics: Clinical Assessment and Imaging
A qualified healthcare professional evaluates lower back pain through a combination of medical history, physical examination, and—when indicated—imaging studies or laboratory tests. Key components of the clinical assessment include:
- History Taking: Documenting pain onset, duration, aggravating/alleviating factors (including rest or movement), and any associated symptoms such as neurological deficit.
- physical Exam: Assessment of ure, spinal mobility, muscle strength, and reflex integrity.
- Imaging: reserved for patients with “red flags” (e.g., unremitting pain, systemic illness, trauma, neurological compromise). Modalities include X-rays, MRI, and CT scans, as described in clinical radiology reviews.
Laboratory evaluation may be performed to exclude infection, inflammatory arthropathy, or neoplasm in atypical presentations.
Consequences of Prolonged Inactivity
Along with immediate pain exacerbation, extended rest or immobility can lead to secondary complications in low back pain sufferers:
| Result | description | Citation |
|---|---|---|
| Physical Deconditioning | Muscles weaken, losing size and function | MedlinePlus |
| Poor Bone Density | Disuse osteopenia may develop with inactivity | NIH |
| Venous Stasis | Increased risk of deep vein thrombosis (DVT) | CDC |
| Psychological Effects | Depression, anxiety, fear avoidance behaviors | Healthline |
therapeutic Approaches: Breaking the Cycle of Pain and Inactivity
Best practice guidelines advise against prolonged bed rest for non-specific low back pain. The NIH and CDC recommend early, graded resumption of activity to mitigate adverse effects of inactivity.Core components of contemporary therapeutic protocols include:
1. Patient education
Informing patients about the physiological mechanisms behind rest-related pain empowers self-management and reduces fear.Evidence suggests that understanding “hurt ≠ harm” decreases reliance on passive treatments and fosters recovery, as outlined by the NICE guidelines.
2. Physical Therapy and Active Rehabilitation
- Exercise Therapy: Restores muscle strength, endurance, and flexibility. Modalities include aerobic conditioning, core stabilization, and stretching, with robust evidence from Cochrane reviews supporting early mobilization over rest.
- Manual Therapy: Techniques such as manipulation and myofascial release may complement active exercise, especially in subgroups with mechanical pain generators.
3.Ergonomic Modification
Optimizing workplace, home, and sleeping environments to support lumbar health is essential. Use of supportive chairs, proper sleeping surfaces, and regular ural breaks reduce strain on lumbar tissues (Mayo Clinic).
4. Pharmacological Management
Analgesics (acetaminophen, NSAIDs), muscle relaxants, and—in select cases—neuropathic pain agents might potentially be indicated for symptom control, but do not replace the need for mobilization, as stressed in pharmacotherapy reviews.
5. Multidisciplinary and Advanced Interventions
- Cognitive Behavioral Therapy (CBT): Effective for patients with chronic pain and psychosocial contributors, as outlined by the JAMA Network.
- Interventional Procedures: Nerve blocks, spinal injections, or surgery may be considered in recalcitrant cases with clear anatomical indications (NHS).
Self-Management Strategies and Preventive Actions
- Stay Active: Incorporate gentle movement upon waking (e.g., light stretching, walking).
- Break Up Inactivity: Avoid sitting or lying for more than 30–60 minutes without movement (Harvard Health).
- Supportive Sleep: Choose mattresses and pillows that maintain spinal alignment.
- Monitor Psychological Well-being: Address depressive and anxiety symptoms related to pain.
Prognosis: Course and outcomes
Most cases of lower back pain resolve within weeks with appropriate care and early mobilization; though, chronicity and recurrence are not uncommon without preventive strategies. Poor adherence to recommended activity,persistent sedentary behaviour,or maladaptive coping can worsen outcomes and lead to chronic disability. Prognosis is generally favorable when evidence-based principles are applied early, per the WHO and CDC.
Frequently Asked Questions (FAQs)
- Q: Should I stay in bed when my lower back hurts?
no. Evidence strongly discourages prolonged bed rest for non-specific low back pain. Gentle movement and gradual resumption of routine activities accelerate recovery and reduce chronicity risk (Mayo Clinic).
- Q: Why do I feel worse in the morning or after sitting?
Pain after rest is typically due to muscle and ligament stiffness, disc swelling, and inflammatory mediator accumulation, all of which improve with gentle mobilisation (Healthline).
- Q: When should I see a doctor about lower back pain?
Seek prompt medical attention if symptoms persist for more than a few weeks, are severe, are associated with nerve symptoms (numbness, tingling, weakness), or follow trauma/injury. Additionally, red flags such as unexplained weight loss, fever, or bowel/bladder disturbance warrant urgent assessment (NIH).
Conclusion
Lower back pain that feels worse after resting too long is a multifaceted problem rooted in biomechanical, inflammatory, neural, and psychosocial mechanisms.Prolonged inactivity, contrary to intuition, frequently enough exacerbates rather than alleviates symptoms due to muscular atrophy, connective tissue rigidity, disc changes, and neural sensitization. Evidence-based management emphasizes education, early mobilization, physical therapy, and patient-centered care, all shown to improve outcomes and reduce recurrence. By understanding and addressing the underlying pathophysiological processes, healthcare providers and patients alike can break the cycle of lower back pain worsening after rest, promoting pain relief, functional restoration, and return to normal life.
For more in-depth, clinically reviewed content and patient support, visit trusted sources such as the Mayo Clinic,NHS, or CDC back pain resources.